Introduction
Tourniquet palsy is a rare but clinically significant complication associated with the use of a tourniquet during surgical procedures, particularly in orthopedic operations. Tourniquets are widely used to create a bloodless surgical field; however, prolonged application or excessive pressure can lead to nerve compression and ischemic injury. Early identification and timely rehabilitation are essential to prevent long-term neurological deficits and restore functional ability.
Definition
Tourniquet palsy is a type of peripheral nerve injury caused by mechanical compression and decreased blood flow to nerves due to prolonged or improperly applied tourniquet pressure. It may result in temporary or, in rare cases, permanent impairment of motor and sensory function in the affected limb.
Clinical Features
The presentation of tourniquet palsy depends on the nerve involved and duration of compression. Common clinical features include:
- Weakness of muscles distal to the site of compression
- Decreased reflexes in the affected limb
- Sensory disturbances such as numbness or tingling
- Difficulty in performing coordinated movements
- Local discomfort or pain following surgery
Symptoms usually appear soon after removal of the tourniquet and may gradually improve with appropriate care.
Signs and Symptoms
Patients with tourniquet palsy may exhibit:
- Muscle weakness or paralysis in the affected region
- Tingling or “pins and needles” sensation
- Loss or reduction of sensation (paresthesia)
- Reduse muscle tone
- Impaired voluntary movements
- Functional limitations in daily activities
- In severe cases, features like wrist drop or foot drop, depending on the nerve involved
These symptoms may vary in severity depending on the extent of nerve injury.
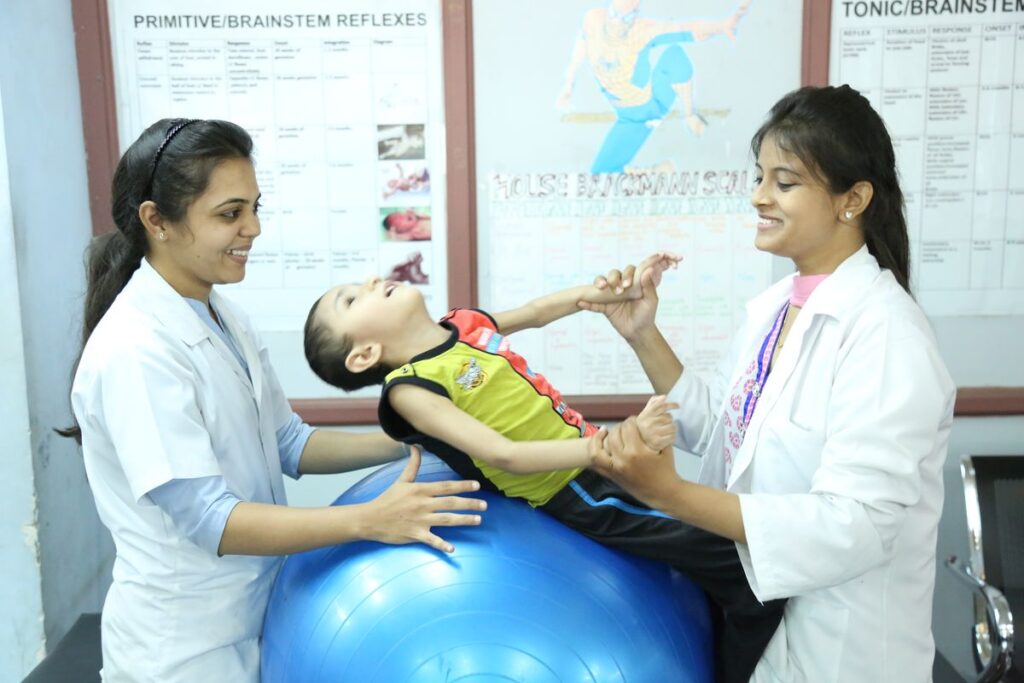
Physiotherapy Management
Physiotherapy plays a vital role in promoting nerve recovery and restoring function. Key management strategies include:
- Muscle Strengthening Exercises: Improve the strength of affected muscle groups
- Range of Motion Exercises: Maintain joint mobility and prevent stiffness
- Nerve Mobilization Techniques: Enhance nerve gliding and decrease adhesions
- Electrical Stimulation: Facilitates muscle activation in cases of weakness
- Functional Training: Restore independence in daily activities
- Sensory Re-education: Improve sensory awareness and coordination
- Patient Education: Encourage gradual return to activity and limb protection
A structured and individualized rehabilitation program is essential for optimal recovery.
Conclusion
Tourniquet palsy is an uncommon but preventable complication of surgical tourniquet use. Although most cases are reversible, early diagnosis and prompt physiotherapy intervention are vital to ensure complete functional recovery. Proper surgical techniques, controlled tourniquet pressure, and postoperative rehabilitation remarkably improve patient outcomes and decrease the risk of long-term disability.
Q: What is tourniquet palsy?
A: It is a peripheral nerve injury caused by prolonged tourniquet pressure leading to nerve compression and reduced blood flow.
Q: What are the common symptoms of tourniquet palsy?
A: Muscle weakness, numbness, tingling, decreased reflexes, and in severe cases, wrist or foot drop.
Q: How is tourniquet palsy managed?
A: Through physiotherapy including strengthening exercises, range of motion, nerve mobilization, and functional training.

